THE 4 STAGES OF SHOCK
Summary
TLDRThis script delves into shock, a critical medical emergency characterized by inadequate tissue perfusion leading to organ damage and potential death. It outlines the physiological response to shock, detailing the four types: hypovolemic, cardiogenic, obstructive, and distributive. The progression through initial, compensatory, progressive, and refractory stages is explained, highlighting the importance of early intervention. The script also describes the body's compensatory mechanisms, such as the sympathetic nervous system activation and the renin-angiotensin system, which aim to maintain blood pressure and perfusion. However, as shock progresses, these mechanisms falter, leading to organ dysfunction and failure. The summary emphasizes the urgency of addressing shock to prevent severe outcomes, noting that hypovolemic shock is most common in children, while septic shock predominates in adults.
Takeaways
- 🚨 Shock is a medical emergency that can lead to organ damage and death due to inadequate tissue perfusion.
- 🔍 Tissue perfusion is essential for delivering oxygen and nutrients to cells and removing waste; ineffective perfusion can cause tissue death.
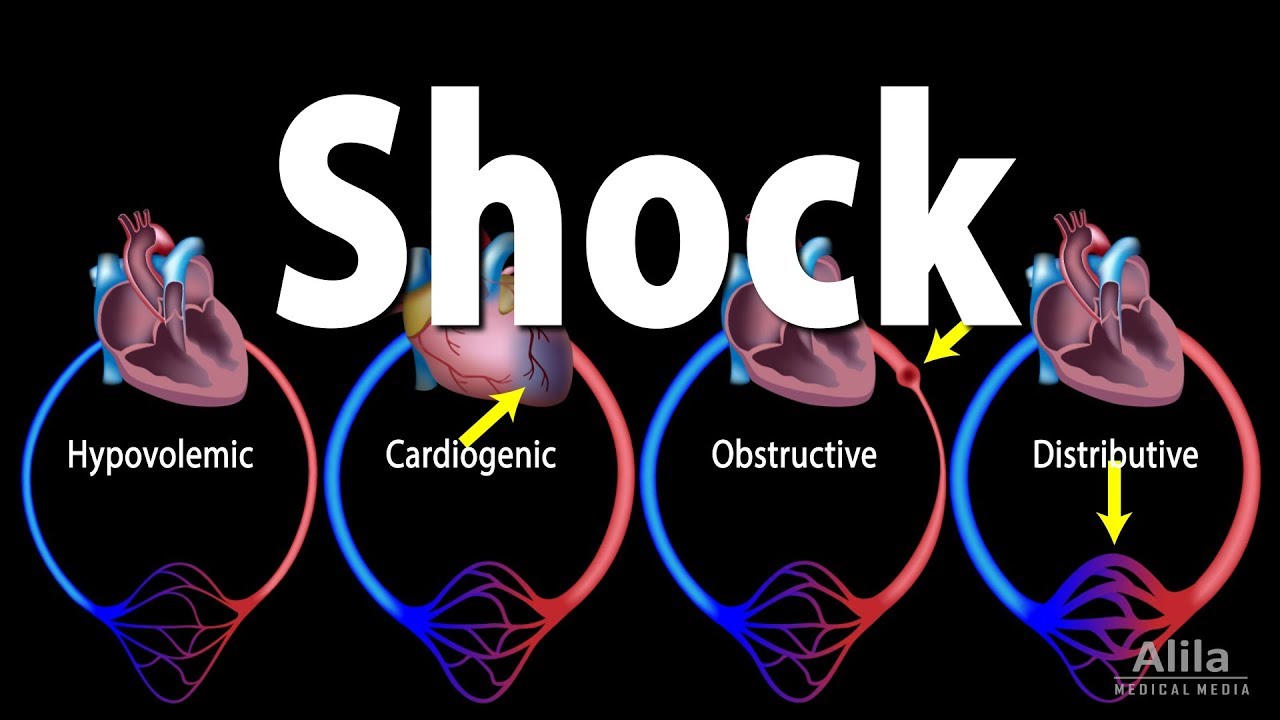
- 🏥 There are four types of shock: hypovolemic, cardiogenic, obstructive, and distributive (including anaphylactic, septic, and neurogenic shock).
- 📈 Shock progresses through four stages: initial, compensatory, progressive, and refractory, with early intervention being crucial.
- 🌡️ In the initial stage, decreased tissue perfusion leads to hypoxia and cells switch from aerobic to anaerobic metabolism, producing lactic acid.
- 🧠 The sympathetic nervous system is activated in response to decreased blood pressure, causing vasoconstriction and increased heart rate.
- 💊 The renin-angiotensin system is triggered to regulate blood pressure and vascular resistance, with angiotensin II being a key vasoconstrictor.
- 🩺 Compensatory mechanisms aim to increase cardiac output and blood volume, but at the cost of decreased perfusion to non-vital organs.
- 🚨 In the progressive stage, compensatory mechanisms fail, leading to worsening tissue damage and progression towards multiple organ dysfunction syndrome.
- 🏥 Organ-specific effects of shock include mental status changes in the brain, cardiac dysrhythmias, respiratory distress syndrome, GI bleeding, and coagulation issues.
- 💔 The refractory stage of shock is characterized by poor tissue perfusion, hypotension, and organ failure, often leading to a fatal outcome.
Q & A
What is shock and why is it considered a medical emergency?
-Shock is a complex physiological response triggered by decreased tissue perfusion, which is the process of blood flowing through the body to provide oxygen and nutrients and remove cellular waste. It is a medical emergency because it can lead to organ damage and death during shock.
What are the four types of shock mentioned in the script?
-The four types of shock are hypovolemic, cardiogenic, obstructive, and distributive. Distributive shock further encompasses anaphylactic, septic, and neurogenic shock.
What happens during the initial stage of shock?
-In the initial stage, also known as the early, non-progressive, or pre-shock stage, there is a decrease in tissue perfusion and cardiac output. Cells begin to experience hypoxia, and anaerobic metabolism starts, leading to a buildup of lactic acid and acidosis.
How does the sympathetic nervous system respond to shock?
-The sympathetic nervous system is stimulated by baroreceptors in the carotid sinus and aortic arch when they sense a drop in blood pressure. It releases catecholamines like epinephrine and norepinephrine, causing vasoconstriction, increased blood pressure, and heart rate.
What is the role of antidiuretic hormone in shock?
-Antidiuretic hormone is released from the posterior pituitary gland in response to stimulation by the vagus nerve. It prevents water from leaving the kidneys, thereby increasing blood volume.
Can you explain the renin-angiotensin system and its function during shock?
-The renin-angiotensin system is a hormone system that regulates fluid and electrolyte balance, blood pressure, and vascular resistance. During shock, it is activated to increase vascular resistance and blood pressure, and it also promotes the retention of sodium and water in the kidneys, increasing blood volume.
What are the consequences of decreased tissue perfusion during the progressive stage of shock?
-During the progressive stage, compensatory mechanisms fail, leading to worsening tissue damage. Cells do not receive oxygen and begin to swell, capillary permeability increases, and fluid and protein are drawn into the interstitial space, resulting in major edema and decreased cardiac output and tissue perfusion.
What happens to the brain and heart during the progressive stage of shock?
-In the progressive stage, inadequate perfusion to the brain can cause major mental status changes, slow speech, agitation, and unresponsiveness to stimulation. In the heart, cells begin to die, including those of the electrical conduction system, leading to cardiac dysrhythmias.
How does the respiratory system respond to decreased blood oxygen levels during shock?
-To compensate for decreased blood oxygen levels, the person hyperventilates, increasing the rate and depth of their breathing. However, in severe cases like acute respiratory distress syndrome, the lungs lose elasticity, fluid accumulates in the lungs, and respiratory failure may occur, requiring intubation and mechanical ventilation.
What are the effects of shock on the gastrointestinal tract and the liver?
-In the gastrointestinal tract, cells begin to die, leading to the formation of ulcers and massive gastrointestinal bleeding. The liver, being involved in clotting factor production, is also affected, leading to disseminated intravascular coagulation and uncontrolled bleeding.
What is the final stage of shock called, and what characterizes it?
-The final stage of shock is called the refractory stage. It is characterized by poor tissue perfusion, hypotension, and organ failure despite aggressive resuscitation efforts, and the person is unlikely to survive.
What are the most common causes of shock in children and adults?
-The most common cause of shock in children is hypovolemic shock, while in adults, it is septic shock.
Outlines

Cette section est réservée aux utilisateurs payants. Améliorez votre compte pour accéder à cette section.
Améliorer maintenantMindmap

Cette section est réservée aux utilisateurs payants. Améliorez votre compte pour accéder à cette section.
Améliorer maintenantKeywords

Cette section est réservée aux utilisateurs payants. Améliorez votre compte pour accéder à cette section.
Améliorer maintenantHighlights

Cette section est réservée aux utilisateurs payants. Améliorez votre compte pour accéder à cette section.
Améliorer maintenantTranscripts

Cette section est réservée aux utilisateurs payants. Améliorez votre compte pour accéder à cette section.
Améliorer maintenant5.0 / 5 (0 votes)