Septic Shock (Sepsis) | Pathophysiology and Nursing Interventions
Summary
TLDRSepsis is a severe systemic infection that begins with bacterial invasion and can lead to multiple organ failure. It results from a dysregulated immune response following a breach in the body's defenses, causing widespread inflammation, blood clotting, low blood pressure, and poor tissue perfusion. Risk factors include infections, wounds, hospitalizations, immune deficiencies, and chronic diseases. Symptoms range from fever and malaise to hypotension, tachycardia, and organ dysfunction. Sepsis progresses through stages, from infection to systemic inflammatory response syndrome (SIRS), severe sepsis, septic shock, and ultimately, multiple organ dysfunction syndrome (MODS), which can lead to death if untreated.
Takeaways
- 🦠 Sepsis is a systemic infection that can lead to multiple organ failure, starting with bacterial invasion.
- 🩸 Sepsis involves a breach in the host's skin or mucous membranes, leading to a dysregulated immune response.
- 🧬 Inflammatory mediators cause vasodilation, increased capillary permeability, and low blood pressure (hypotension).
- 🧪 The immune response triggers the coagulation cascade and leads to clotting in blood vessels, resulting in poor tissue perfusion and damage.
- 🚨 Risk factors for sepsis include wounds, infections, ICU admission, immune system deficiencies, surgeries, indwelling medical devices, and extremes of age.
- ⚠️ Early signs of sepsis are non-specific, including malaise, fever, hypotension, tachycardia, edema, and hypoxemia.
- 🔬 Lab results show increased white blood cell count, inflammatory markers, serum lactate, and markers of organ damage, with positive blood cultures.
- 💉 Sepsis occurs on a continuum, starting with infection and potentially progressing to systemic inflammatory response syndrome (SIRS), then severe sepsis, septic shock, and multiple organ dysfunction syndrome (MODS).
- 📊 SIRS is diagnosed when two or more criteria are met (e.g., abnormal temperature, heart rate, respiratory rate, or white blood cell count).
- 💀 If untreated, sepsis can result in multiple organ dysfunction and death, with symptoms like respiratory failure, liver and kidney impairment, and cardiac arrest.
Q & A
What is sepsis?
-Sepsis is a continuum of systemic or widespread infection in the bloodstream that starts with bacterial invasion and can lead to multiple organ failure. It is characterized by a dysregulated immune response in the host.
How does sepsis begin?
-Sepsis often begins with a breach in the host's barrier, such as the skin or mucous membranes, which triggers a dysregulated immune response. This response involves inflammatory mediators, vasodilation, increased capillary permeability, and activation of the coagulation and complement cascades.
What are some common risk factors for sepsis?
-Risk factors for sepsis include wounds (pressure injuries, traumatic wounds, chronic non-healing wounds), infections (such as kidney or lung infections), hospital or ICU admission, immune system deficiencies (HIV, cancer), recent surgeries, indwelling medical devices (central lines, urinary catheters), very young or old age, chronic disease, and genetics.
What are the early symptoms of sepsis?
-Early symptoms of sepsis include general, non-specific signs such as malaise and fever. As sepsis progresses, hypotension and tachycardia may develop due to vasodilation and increased capillary permeability.
How does the immune response in sepsis lead to tissue damage?
-In sepsis, the immune system releases pro-inflammatory mediators that cause detrimental effects such as clotting in the blood vessels. This clotting blocks blood flow, leading to poor tissue perfusion and tissue damage.
What laboratory markers are elevated in sepsis?
-Laboratory markers in sepsis include an increased white blood cell count (with immature white blood cells indicating a left shift), increased inflammatory markers such as C-reactive protein and erythrocyte sedimentation rate, and markers of hypoperfusion such as elevated serum lactate.
What are the clinical manifestations of sepsis as it progresses?
-As sepsis progresses, clinical manifestations include hypotension, tachycardia, edema, tachypnea, hypoxemia, and low urine output due to poor perfusion and kidney damage. Signs of organ damage such as increased creatinine and bilirubin levels may also be seen.
What is Systemic Inflammatory Response Syndrome (SIRS), and how is it related to sepsis?
-SIRS is a widespread inflammatory reaction that can occur as a response to infection or other inflammatory causes. Sepsis is diagnosed when SIRS criteria are met, and there is a diagnosed source of infection. SIRS involves two or more symptoms, including abnormal temperature, heart rate, respiratory rate, and white blood cell count.
What differentiates severe sepsis from septic shock?
-Severe sepsis is characterized by hypotension or hypoperfusion, leading to lactic acidosis and organ dysfunction. Septic shock occurs when hypotension persists despite adequate fluid resuscitation, indicating more severe circulatory failure.
What is Multiple Organ Dysfunction Syndrome (MODS), and how is it related to sepsis?
-MODS occurs when septic shock leads to the failure of two or more organs, such as respiratory failure, liver impairment, kidney impairment, neurological impairment, and cardiac impairment. If left untreated, MODS can result in death.
Outlines

Esta sección está disponible solo para usuarios con suscripción. Por favor, mejora tu plan para acceder a esta parte.
Mejorar ahoraMindmap

Esta sección está disponible solo para usuarios con suscripción. Por favor, mejora tu plan para acceder a esta parte.
Mejorar ahoraKeywords

Esta sección está disponible solo para usuarios con suscripción. Por favor, mejora tu plan para acceder a esta parte.
Mejorar ahoraHighlights

Esta sección está disponible solo para usuarios con suscripción. Por favor, mejora tu plan para acceder a esta parte.
Mejorar ahoraTranscripts

Esta sección está disponible solo para usuarios con suscripción. Por favor, mejora tu plan para acceder a esta parte.
Mejorar ahoraVer Más Videos Relacionados
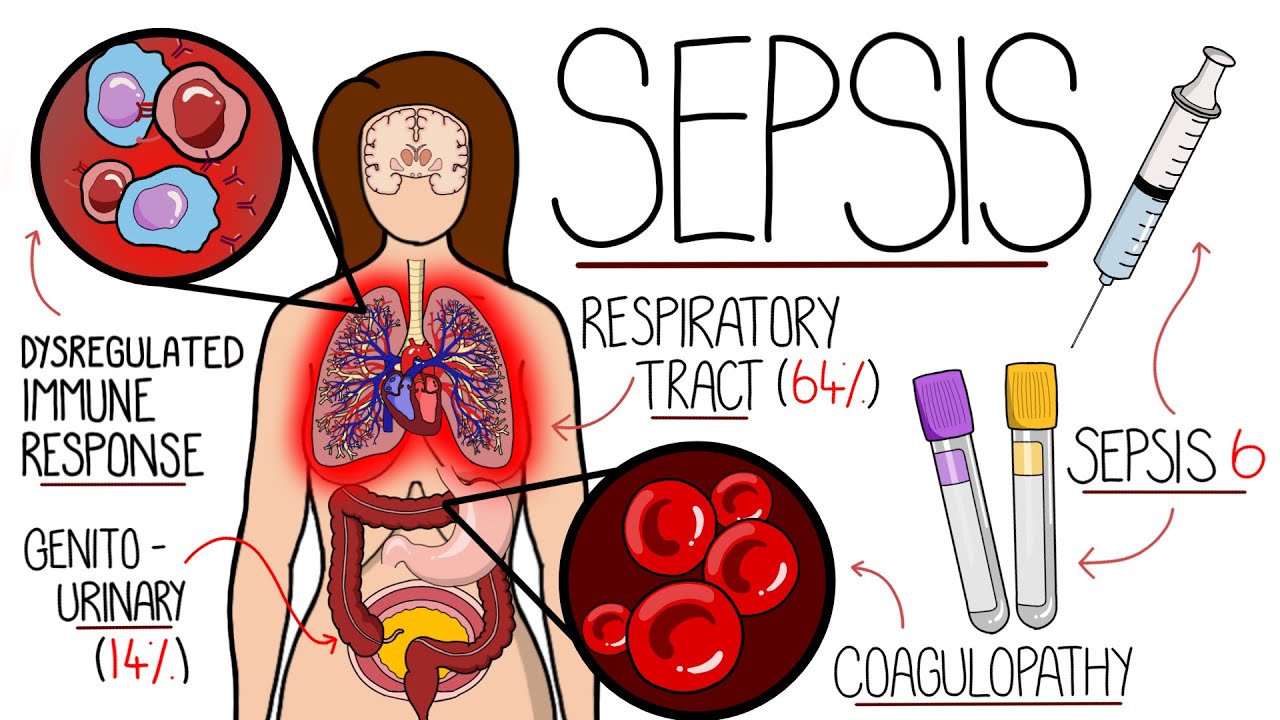
Understanding Sepsis (Sepsis Explained Clearly)

Understanding Sepsis & Septic Shock (Visual Guide) | 2024 Updated Tutorial
Sepsis and Septic Shock, Animation.

Leptospirosis, Causes, Signs and Symptoms, Diagnosis and Treatment

SEPSIS PATHOPHYSIOLOGY IN 7 SIMPLE STEPS (2018)

Peritonsillar abscess (mechanism of disease)
5.0 / 5 (0 votes)
