Type II hypersensitivity (cytotoxic hypersensitivity) - causes, symptoms, & pathology
Summary
TLDRThe video script delves into type II hypersensitivity, a condition where the immune system mistakenly attacks healthy cells. It explains how antibodies, particularly IgG and IgM, can lead to tissue damage through mechanisms like complement system activation, cell lysis, and antibody-dependent cell-mediated cytotoxicity. The script also touches on non-cytotoxic effects and diagnostics like the Coomb’s test, highlighting the specificity and potential severity of this immune response.
Takeaways
- 🚨 Hypersensitivity refers to the immune system's overreaction to substances, causing harm instead of protection.
- 🔍 There are four types of hypersensitivities, with Type II, or cytotoxic hypersensitivity, involving antibody-mediated destruction of healthy cells.
- 🏠 Type II hypersensitivity disorders are often tissue-specific, with antibodies targeting a specific tissue or organ.
- 🌐 Type III hypersensitivities are systemic and involve antibody-antigen complexes causing widespread inflammation.
- 🛡️ Central tolerance is a process that eliminates self-reactive immune cells during their development in primary lymphoid organs.
- 🚫 Some self-reactive B and T cells escape central tolerance and can lead to autoimmune diseases.
- 🏥 In Type II hypersensitivity, self-reactive B cells produce antibodies that attach to antigens on host cells, which can be intrinsic or extrinsic.
- 💊 Medications like penicillin can act as extrinsic antigens, binding to host cells and triggering an immune response.
- 🩸 The complement system is activated in Type II hypersensitivity, leading to the destruction of cells bound to the antigen-antibody complex.
- 🧬 The direct Coomb’s test is used to detect antibodies on red blood cells in conditions like autoimmune hemolytic anemia.
- 🔄 Non-cytotoxic Type II hypersensitivities can disrupt cell function rather than causing cell death, as seen in diseases like Myasthenia gravis and Grave’s disease.
Q & A
What is hypersensitivity and how does it differ from a normal immune response?
-Hypersensitivity refers to an immune system reaction that damages the body instead of protecting it. Unlike a normal immune response that targets 'non-self' entities, hypersensitivity involves the immune system mistakenly reacting to substances that are not harmful, leading to adverse effects on the body's own tissues.
How many types of hypersensitivities are there, and what is Type II hypersensitivity?
-There are four types of hypersensitivities. Type II hypersensitivity, also known as cytotoxic hypersensitivity, involves the destruction of healthy cells by antibodies, often targeting specific tissues or organs.
What is the role of central tolerance in preventing autoimmune diseases?
-Central tolerance is a process during which self-reactive immune cells are destroyed or inactivated while they are still in the primary lymphoid organs, such as the thymus for T cells and bone marrow for B cells. This helps to prevent autoimmune diseases by eliminating cells that could potentially attack the body's own tissues.
How do self-reactive B cells contribute to Type II hypersensitivity?
-In Type II hypersensitivity, self-reactive B cells that have escaped central tolerance become activated and produce antibodies like IgM or IgG, which attach to antigens on host cells, leading to tissue damage or autoimmune disease.
What are the two types of antigens involved in Type II hypersensitivity?
-The two types of antigens involved in Type II hypersensitivity are intrinsic antigens, which are normally produced by the host cell, and extrinsic antigens, which come from external sources like infections or medications, such as penicillin.
Can you explain the cytotoxic mechanism involving the complement system in Type II hypersensitivity?
-The complement system is activated by IgG or IgM antibodies binding to antigens on host cells. This activation leads to a cascade of events involving complement proteins, ultimately resulting in the destruction of the host cell, such as a red blood cell bound to penicillin.
What is the difference between the direct and indirect Coomb’s test?
-The direct Coomb’s test detects antibodies on the surface of red blood cells, indicating an autoimmune response. The indirect Coomb’s test checks for the presence of antibodies or complement in the serum that could cause agglutination with known antigens on laboratory red blood cells, and is used to determine pre-existing antibodies, such as in blood group incompatibility.
How does the membrane attack complex (MAC) contribute to cell lysis in Type II hypersensitivity?
-The MAC, formed by complement proteins C5b, C6-C8, and multiple C9 molecules, inserts itself into the cell membrane, creating a channel that allows fluid and molecules to flow in and out. This leads to cell swelling and eventual lysis, causing cell death.
What is opsonization and how does it relate to Type II hypersensitivity?
-Opsonization is the process where cells are marked for phagocytosis by having antibodies or complement proteins bound to their surface. In Type II hypersensitivity, opsonized cells are targeted and destroyed by phagocytes like macrophages and neutrophils.
Can you describe antibody-dependent cell-mediated cytotoxicity (ADCC) in the context of Type II hypersensitivity?
-ADCC is a mechanism where natural killer cells recognize the Fc tail of antibodies bound to antigens on host cells and release toxic granules containing perforins and granzymes. These substances induce cell death through apoptosis, a process that does not cause inflammation.
What are non-cytotoxic Type II hypersensitivities and how do they differ from cytotoxic ones?
-Non-cytotoxic Type II hypersensitivities involve antibodies binding to antigens in a way that disrupts cell function rather than causing cell death. Examples include Myasthenia gravis, where antibodies block the acetylcholine receptor, and Grave’s disease, where antibodies activate receptors, leading to cellular dysfunction.
Outlines

このセクションは有料ユーザー限定です。 アクセスするには、アップグレードをお願いします。
今すぐアップグレードMindmap

このセクションは有料ユーザー限定です。 アクセスするには、アップグレードをお願いします。
今すぐアップグレードKeywords

このセクションは有料ユーザー限定です。 アクセスするには、アップグレードをお願いします。
今すぐアップグレードHighlights

このセクションは有料ユーザー限定です。 アクセスするには、アップグレードをお願いします。
今すぐアップグレードTranscripts

このセクションは有料ユーザー限定です。 アクセスするには、アップグレードをお願いします。
今すぐアップグレード関連動画をさらに表示

gangguan pada sistem imun/ sistem pertahanan tubuh - biologi sma kelas 11 semester 2 bab.sistem imun

Hypersensitivity, Overview of the 4 Types, Animation.

Type III hypersensitivity (immune complex mediated) - causes, symptoms & pathology

Hipersensitivitas Tipe 1 (Immediate Hypersensitivity), Immunology
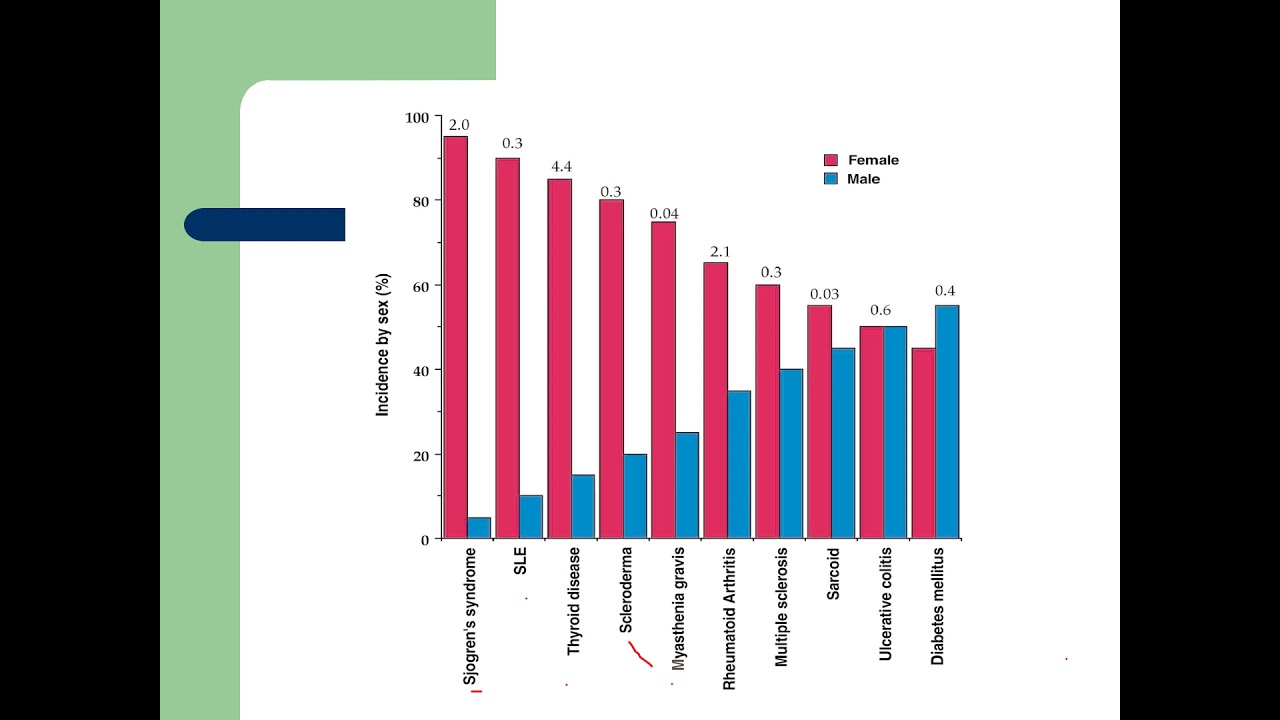
Autoimunidade

Hypersensitivity Part II|Simplified Explanation|Immunology|Allergy|Immune System|IgG & IgM Antibody|
5.0 / 5 (0 votes)
