Understanding the Menstrual Cycle
Summary
TLDRThis video provides a clear and straightforward explanation of the menstrual cycle, focusing on the roles of four main hormones: FSH, LH, estrogen, and progesterone. It describes the two phases of the cycle—follicular and luteal—highlighting how hormone levels fluctuate to regulate ovulation, menstruation, and the endometrial lining. The speaker also explains the role of key structures like the hypothalamus, pituitary gland, and ovaries, while offering insights into how pregnancy affects hormone production. The video serves as a helpful resource for medical students and anyone interested in understanding the menstrual cycle.
Takeaways
- 🧠 The menstrual cycle is regulated by four main hormones: FSH (Follicle Stimulating Hormone), LH (Luteinizing Hormone), estrogen, and progesterone.
- 🗓️ The menstrual cycle typically lasts 28 days and consists of two phases: the follicular phase (first 14 days) and the luteal phase (last 14 days).
- 🥚 The follicular phase involves the development of an egg within a follicle, while the luteal phase begins after ovulation, when the egg has exited the ovary and the corpus luteum forms.
- 📏 The length of the follicular phase can vary, affecting the overall length of the cycle, but the luteal phase is consistently 14 days long.
- 🧬 The hypothalamus and anterior pituitary gland play key roles in initiating the cycle by releasing hormones that stimulate the ovaries.
- 🔄 Estrogen, released by developing follicles, promotes the thickening of the uterine lining and prepares the body for possible pregnancy.
- 📈 LH spikes right before ovulation, causing the release of the egg from the ovary around day 14 of the cycle.
- 💊 After ovulation, the corpus luteum produces progesterone, which helps maintain the uterine lining and supports early pregnancy if fertilization occurs.
- ❌ If fertilization doesn't happen, the corpus luteum breaks down, causing a drop in estrogen and progesterone, leading to the shedding of the uterine lining (menstruation).
- 🔁 The cycle restarts as FSH levels rise again after menstruation, stimulating the next batch of follicles.
Q & A
What are the four main hormones involved in the menstrual cycle?
-The four main hormones involved in the menstrual cycle are follicle stimulating hormone (FSH), luteinizing hormone (LH), estrogen, and progesterone.
How long is a typical menstrual cycle and how are its phases divided?
-A typical menstrual cycle is 28 days long, divided into two phases of 14 days each. The first phase is the follicular phase, and the second phase is the luteal phase.
Why is the luteal phase always 14 days long regardless of the cycle length?
-The luteal phase is always 14 days long because it is determined by the lifespan of the corpus luteum, which remains constant. If the cycle is shorter, the follicular phase is shorter, and if it's longer, the follicular phase is longer.
What are the key structures in the body that release hormones related to the menstrual cycle?
-The key structures are the hypothalamus and the pituitary gland in the brain, and the pelvic organs including the ovaries, which release hormones that regulate the menstrual cycle.
What is the role of the endometrium in the menstrual cycle?
-The endometrium is the lining of the uterus that provides a supportive environment for a fertilized egg to implant. It breaks down and bleeds every month during menstruation to be renewed for a new cycle.
How does the hypothalamus initiate the menstrual cycle?
-The hypothalamus initiates the menstrual cycle by releasing gonadotropin-releasing hormone (GnRH), which stimulates the anterior pituitary gland to release FSH and LH.
What happens to the follicles during the follicular phase?
-During the follicular phase, FSH stimulates the development of 15 to 20 primordial follicles within the ovaries, and as they develop, they secrete increasing amounts of estrogen.
What causes the surge in luteinizing hormone (LH) that leads to ovulation?
-A dip in estrogen levels just before ovulation triggers a surge in LH, which causes one of the follicles to release the ovum or unfertilized egg.
What is the function of the corpus luteum after ovulation?
-After ovulation, the follicle that released the ovum collapses and becomes the corpus luteum, which secretes high levels of progesterone and some estrogen to maintain and thicken the endometrial lining.
What happens if the ovum is not fertilized?
-If the ovum is not fertilized, the corpus luteum degenerates, stopping the production of progesterone and estrogen. This drop in hormone levels leads to the breakdown of the endometrium and the start of menstruation.
How does menstruation occur and what is its duration?
-Menstruation occurs when the levels of estrogen and progesterone drop, causing the endometrium to break down. The tissue is shed through the cervix and vagina, causing bleeding that lasts between one and eight days.
Outlines

此内容仅限付费用户访问。 请升级后访问。
立即升级Mindmap

此内容仅限付费用户访问。 请升级后访问。
立即升级Keywords

此内容仅限付费用户访问。 请升级后访问。
立即升级Highlights

此内容仅限付费用户访问。 请升级后访问。
立即升级Transcripts

此内容仅限付费用户访问。 请升级后访问。
立即升级浏览更多相关视频
CICLO MENSTRUAL (FISIOLOGIA DE GUYTON) - MENSTRUAÇÃO - FISIOLOGIA HUMANA - OVULAÇÃO

Female Reproductive Cycle | Ovulation & Menstrual Cycle: Overview

Lesson 4: The Feedback Mechanism in Menstrual Cycle
CICLO MENSTRUAL COMPLETO (FISIOLOGIA DE GUYTON) - MENSTRUAÇÃO - FISIOLOGIA HUMANA - OVULAÇÃO

Ciclo Menstrual - Aula 35 - Módulo VII: Fisiologia Humana | Prof. Gui
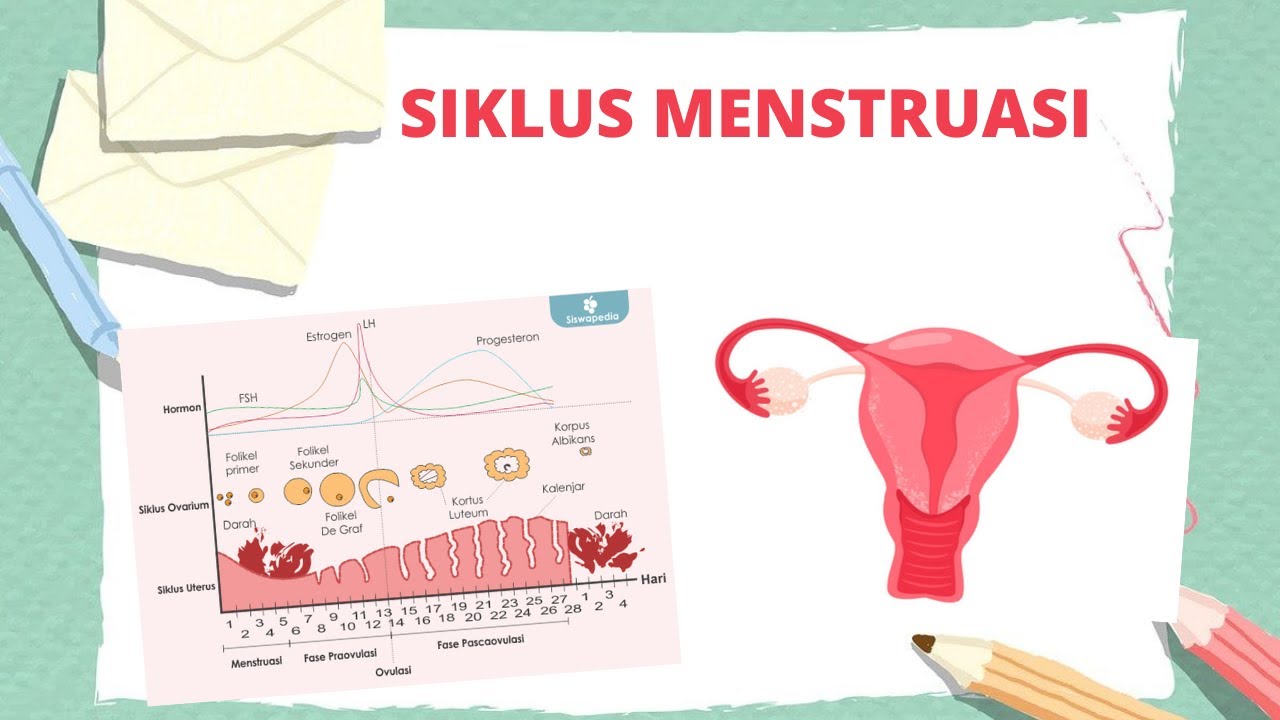
Siklus menstruasi - Grafik siklus menstruasi dan penjelasannya
5.0 / 5 (0 votes)
