Aminoglycosides Pharmacology Nursing Antibiotics: Mechanism of Action, Mnemonic, Anti-Infectives
Summary
TLDRThis video covers aminoglycosides, a group of antibiotics primarily targeting gram-negative bacteria. They have a bactericidal effect, making them effective for infections like septicemia, UTIs, and pneumonia. Aminoglycosides inhibit protein synthesis by binding to the 30S ribosomal subunit. They're often used with other antibiotics, like penicillin, for a synergistic effect. The video discusses key drugs in this class, how they're administered, and the importance of monitoring for nephrotoxicity, ototoxicity, and neuromuscular issues, emphasizing the need for careful patient monitoring to avoid adverse effects.
Takeaways
- 💊 Aminoglycosides are antibiotics primarily targeting gram-negative bacteria, with bactericidal effects that kill the bacteria rather than just inhibiting its growth.
- 🦠 These antibiotics are effective against bacteria like E. coli, Klebsiella pneumoniae, Pseudomonas aeruginosa, and Serratia marcescens, but have limited effectiveness against gram-positive bacteria.
- 🧬 Aminoglycosides work by inhibiting protein synthesis in bacterial cells by targeting the 30S ribosomal subunit, leading to faulty protein production and bacterial death.
- 💉 Aminoglycosides are usually administered via the IM or IV route, as they are poorly absorbed through the gut, though certain exceptions exist (e.g., neomycin for gut infections).
- 🧪 Peak and trough levels should be closely monitored due to the narrow therapeutic index, ensuring the drug is effective while avoiding toxicity.
- 🚨 Nephrotoxicity (kidney damage) and ototoxicity (hearing damage) are major risks of aminoglycosides, requiring careful monitoring of renal function and hearing.
- 🔬 In some cases, aminoglycosides are combined with other antibiotics like penicillin for a synergistic effect, improving their ability to penetrate bacterial cells.
- 👂 Ototoxicity, or damage to the ears, is usually irreversible and may present as tinnitus, hearing loss, or dizziness, particularly in patients also taking loop diuretics.
- 🫁 Neuromuscular blockade, leading to muscle weakness or respiratory failure, is another rare but serious side effect, especially in patients with neuromuscular conditions.
- 🧴 The mnemonic 'GNATS' helps remember the main aminoglycosides: Gentamicin, Neomycin, Amikacin, Tobramycin, and Streptomycin.
Q & A
What types of bacteria do aminoglycosides primarily target?
-Aminoglycosides primarily target gram-negative microorganisms such as E. coli, Klebsiella pneumonia, Pseudomonas aeruginosa, Serratia marcescens, and Enterobacter. They are less effective against gram-positive bacteria but can target some, like Staphylococcus aureus.
How do aminoglycosides kill bacteria?
-Aminoglycosides work by inhibiting protein synthesis in bacteria. They bind to the 30S subunit of the bacterial ribosome, disrupting the genetic code's reading, leading to the production of faulty proteins, which ultimately causes bacterial death.
Why are aminoglycosides often used in combination with other antibiotics?
-Aminoglycosides are used with other antibiotics, like Penicillin, for a synergistic effect. Penicillin helps aminoglycosides penetrate bacterial cell walls more effectively, enhancing their ability to kill bacteria.
What is the mnemonic to remember common aminoglycoside medications?
-The mnemonic to remember aminoglycosides is 'GNATS': G for Gentamicin, N for Neomycin, A for Amikacin, T for Tobramycin, and S for Streptomycin.
How are aminoglycosides typically administered?
-Aminoglycosides are usually administered via intramuscular (IM) or intravenous (IV) routes because they are not well-absorbed through the gut. Exceptions include Tobramycin for inhalation in cystic fibrosis patients and Neomycin for oral use in specific conditions like hepatic encephalopathy.
What conditions can aminoglycosides effectively treat?
-Aminoglycosides are used to treat septicemia, severe urinary tract infections, infections of the eyes, ears, bones, abdomen, pelvis, endocarditis, and hospital-acquired pneumonia. They can also target mycobacterial infections such as tuberculosis.
Why is monitoring peak and trough levels important when administering aminoglycosides?
-Monitoring peak and trough levels ensures the medication is at a therapeutic level to effectively treat the infection while avoiding toxicity. Peak levels are monitored for effectiveness, and trough levels are monitored to prevent toxic accumulation in the body.
What are the major toxic effects of aminoglycosides?
-Aminoglycosides can cause nephrotoxicity (kidney damage) and ototoxicity (hearing damage). Nephrotoxicity is often reversible, but ototoxicity, affecting hearing and balance, is usually permanent.
How can aminoglycosides lead to neuromuscular blockade?
-Aminoglycosides can cause neuromuscular blockade, leading to muscle weakness and respiratory failure, especially in patients with neuromuscular disorders or those who have received neuromuscular blocking medications during anesthesia.
What signs should nurses monitor to ensure aminoglycosides are effectively treating an infection?
-Nurses should monitor for signs like the resolution of fever, normal blood pressure and heart rate, and normal white blood cell count (5,000-10,000 cells/mcL). These indicators suggest that the infection is being effectively treated.
Outlines

Этот раздел доступен только подписчикам платных тарифов. Пожалуйста, перейдите на платный тариф для доступа.
Перейти на платный тарифMindmap

Этот раздел доступен только подписчикам платных тарифов. Пожалуйста, перейдите на платный тариф для доступа.
Перейти на платный тарифKeywords

Этот раздел доступен только подписчикам платных тарифов. Пожалуйста, перейдите на платный тариф для доступа.
Перейти на платный тарифHighlights

Этот раздел доступен только подписчикам платных тарифов. Пожалуйста, перейдите на платный тариф для доступа.
Перейти на платный тарифTranscripts

Этот раздел доступен только подписчикам платных тарифов. Пожалуйста, перейдите на платный тариф для доступа.
Перейти на платный тарифПосмотреть больше похожих видео

Antibiotics classes and coverage in 7 minutes!!

The Gram Stain (Gram-Positive vs Gram-Negative) and Bacterial Structure | Microbiology 🧫

Fluoroquinolones (Quinolones) Pharmacology Nursing Mnemonic, Mechanism of Action NCLEX

BAKTERI GRAM POSITIF DAN BAKTERI GRAM NEGATIF

Cephalosporins Antibiotics Nursing: Mechanism of Action, Pharmacology, Mnemonic, Generations NCLEX
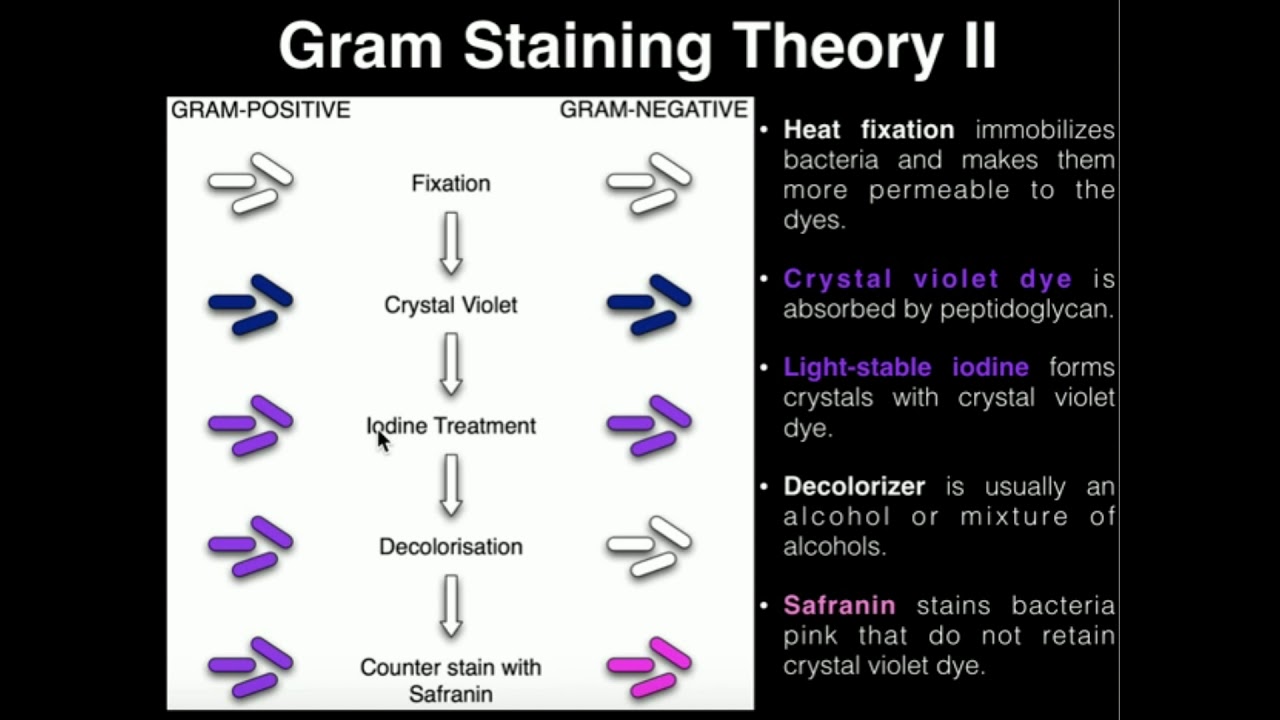
Microbiology: Gram Staining
5.0 / 5 (0 votes)
