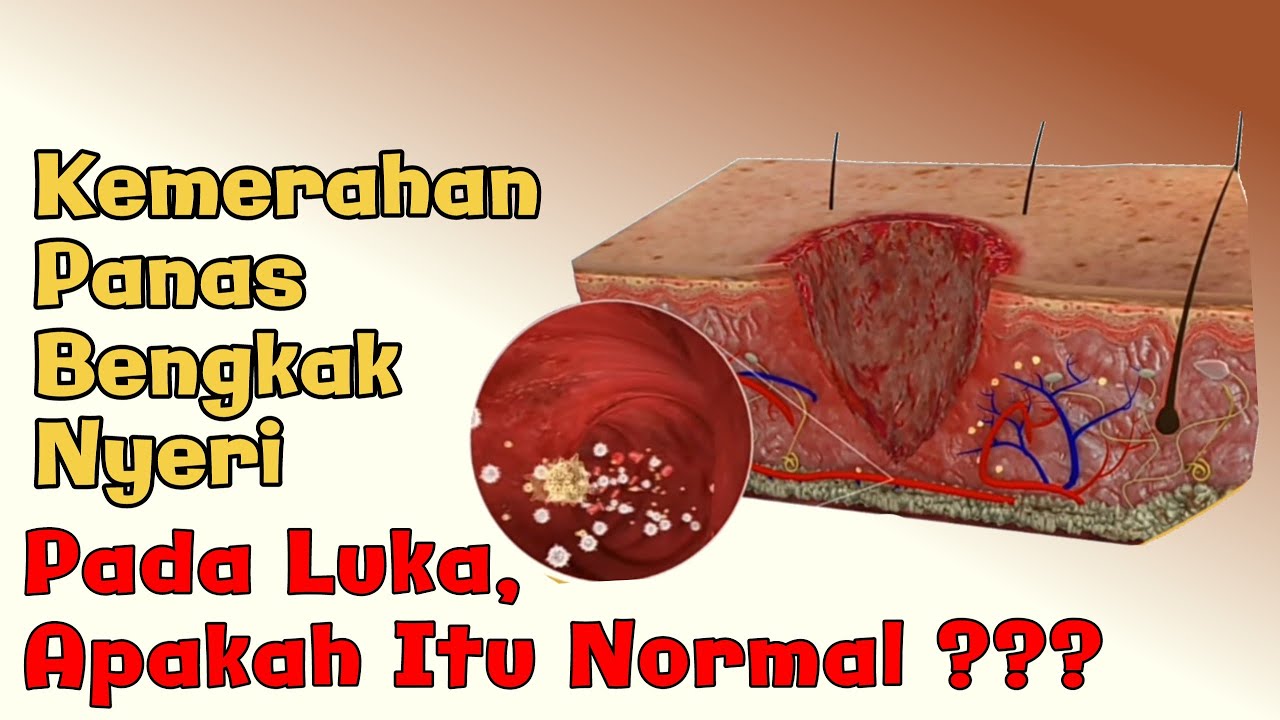
Wound Healing
Summary
TLDRThis video script delves into the intricate phases of wound healing, beginning with the immediate response to injury, which includes vasoconstriction and clot formation. It then details the inflammatory phase, characterized by increased vascular permeability and the action of neutrophils and macrophages. The proliferation phase is highlighted by granulation tissue formation and the activity of fibroblasts. Finally, the script describes wound contraction, re-epithelialization, and the remodeling process that strengthens the wound, potentially taking up to two years to complete.
Takeaways
- 🩸 The initial response to injury involves vasoconstriction to minimize bleeding and the formation of a clot by platelets and red blood cells.
- 🔍 Inflammation begins with the dilation of capillaries, allowing serum and white blood cells to enter the wound site.
- 🔬 White blood cells differentiate into neutrophils and macrophages, which are attracted to damaged cells and bacteria to engulf and remove them.
- 🌡️ The inflammatory phase subsides once dead tissue and bacteria are cleared from the wound.
- 🌱 The proliferation phase is characterized by the formation of granulation tissue, which includes new capillaries and connective tissue.
- 🌿 Angiogenesis, the formation of new capillaries, is crucial for supplying nutrients to the wound and for healing.
- 🧬 Fibroblasts are key cells in the proliferation phase, migrating into the wound to multiply and produce collagen.
- 🔗 Wound contraction occurs in the proliferation phase, facilitated by specialized fibroblasts known as myofibroblasts.
- 🛡️ Re-epithelialization involves epithelial cells changing shape and migrating to cover the wound bed, sealing the wound.
- 🔄 The final stage of wound healing involves the remodeling of collagen fibers, which can take up to two years to maximize tensile strength and form a strong scar.
Q & A
What is the immediate reaction to an injury in the body?
-The immediate reaction to injury is the contraction of capillaries to reduce bleeding, followed by the aggregation of red blood cells and platelets to form a clot in the wound.
What is the role of dilatation of capillaries in the wound healing process?
-Dilatation of capillaries increases permeability, allowing serum and white blood cells to migrate into the wound area, which is essential for the inflammatory process.
How do neutrophils and macrophages contribute to the wound healing process?
-Neutrophils and macrophages are attracted to damaged cells and bacteria by chemical substances. They become phagocytic, engulfing dead tissue and bacteria to clean the wound.
What is the function of granulation tissue in wound healing?
-Granulation tissue, consisting of newly formed capillaries and connective tissue, fills the wound. It ensures nutrient supply for tissue formation and is crucial for wound healing.
What is the role of angiogenesis in the proliferation phase of wound healing?
-Angiogenesis, the formation of new capillaries, is essential for supplying nutrients to the granulation tissue and is vital for wound healing.
What are fibroblasts and how do they contribute to the proliferation phase of wound healing?
-Fibroblasts are the predominant cells in the proliferation phase. They migrate into the wound site, multiply, and produce collagen to rebuild the tissue.
What is wound contraction and how does it occur?
-Wound contraction is the process where the wound is made smaller, brought about by specialized fibroblasts with contractile properties called myofibroblasts.
How does re-epithelialization contribute to wound closure?
-Re-epithelialization involves epithelial cells changing shape to crawl across the wound bed, covering it. Migration stops once cells regain contact, and they reattach to the basement membrane, closing the wound.
What is the final step in the wound healing process described in the script?
-The final step is the transition from granulation tissue to scar tissue, which involves the reorganization and maturation of collagen fibers to maximize tensile strength. This remodeling process can take up to two years.
How long can the remodeling phase of wound healing take?
-The remodeling phase, where collagen fibers are oriented and cross-linked to form a strong wound, can take up to two years after wounding.
Outlines

Этот раздел доступен только подписчикам платных тарифов. Пожалуйста, перейдите на платный тариф для доступа.
Перейти на платный тарифMindmap

Этот раздел доступен только подписчикам платных тарифов. Пожалуйста, перейдите на платный тариф для доступа.
Перейти на платный тарифKeywords

Этот раздел доступен только подписчикам платных тарифов. Пожалуйста, перейдите на платный тариф для доступа.
Перейти на платный тарифHighlights

Этот раздел доступен только подписчикам платных тарифов. Пожалуйста, перейдите на платный тариф для доступа.
Перейти на платный тарифTranscripts

Этот раздел доступен только подписчикам платных тарифов. Пожалуйста, перейдите на платный тариф для доступа.
Перейти на платный тарифПосмотреть больше похожих видео
5.0 / 5 (0 votes)