General Ventilator Set-up by N. McGowan | OPENPediatrics
Summary
TLDRIn this instructional video, Nancy Craig, a Respiratory Therapist at Children's Hospital Boston, provides a comprehensive guide to general ICU ventilator setup. She walks viewers through attaching ventilator components, performing high-pressure leak tests, setting initial ventilator parameters based on patient size, and monitoring end-tidal CO2. The video also covers alarm settings, patient assessment, and ongoing monitoring to ensure safe mechanical ventilation. Finally, it explains proper disassembly and cleaning of the ventilator after use. This practical overview equips healthcare providers with the essential knowledge and step-by-step procedures for safe and effective ventilator management in critically ill patients.
Takeaways
- 🫁 ICU ventilators require proper assembly before patient use, including connecting the inspiratory and expiratory tubing, humidifier, and filters.
- ⚡ Ventilators need a power source and a high-pressure oxygen supply; some models include an air compressor to avoid the need for high-pressure air.
- 🔍 A high-pressure leak test (EST) should be performed before patient use to ensure the circuit has no leaks and oxygen sensors are functioning correctly.
- ⚖️ Initial ventilator settings, such as PIP, PEEP, breath rate, and inspiratory time, are based on patient size and the pressure needed to move the chest.
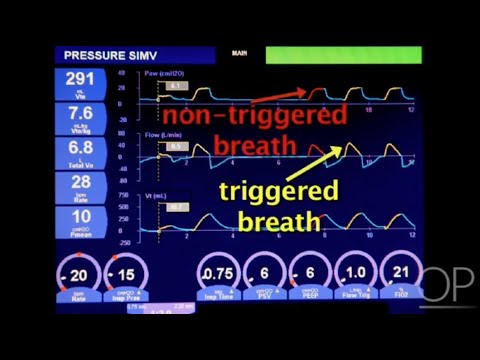
- 💨 Pressure support and flow triggers can be added to assist spontaneous breathing in intubated patients.
- 🧪 End-tidal CO2 monitoring is crucial to assess airway integrity, verify exhalation, and monitor patient ventilation non-invasively.
- 👀 Initial patient assessment involves checking chest rise and ensuring tidal volumes meet target ranges (typically 8-10 cc/kg).
- -
- 🚨 Ventilator alarms (high/low respiratory rate, minute ventilation, peak pressure, apnea interval, and end-tidal CO2) should be set to detect changes in patient status promptly.
- -
- 📊 Regular monitoring of ventilator parameters, breath sounds, airway position, heart rate, blood pressure, and oxygen saturation is necessary to ensure patient safety.
- -
- 🧼 After extubation, ventilators must be disassembled, disposable parts discarded, non-disposable parts cleaned, and the unit sanitized for future use.
Q & A
What are the essential components attached to an ICU ventilator before patient use?
-The essential components include the expiratory filter, the humidifier, inspiratory and expiratory tubing (disposable or non-disposable), a temperature probe for the humidifier, and connections to oxygen and air sources.
Why is a high-pressure leak test (EST) performed when setting up a ventilator?
-The EST ensures that there are no leaks in the ventilator circuit, checks the circuit compliance (distensibility of the tubing), and verifies the functionality of the oxygen sensor. Passing this test confirms the ventilator is safe for patient use.
How does the ventilator use patient weight in initial settings?
-The ventilator uses patient weight to calculate tidal volumes and other parameters to appropriately set the initial ventilatory support, ensuring the patient receives the correct volume per breath.
What initial settings are recommended for a newly intubated patient in pressure control mode?
-Typical initial settings include starting PIP at the pressure required to move the chest (e.g., 25 cmH2O), PEEP around 5 cmH2O, breath rate based on patient size (e.g., 18 breaths/min for a small patient), inspiratory time of 0.5–0.8 seconds, a small amount of pressure support, and an FiO2 of 100%.
What is the purpose of attaching an end-tidal CO2 monitor to the ventilator circuit?
-The end-tidal CO2 monitor non-invasively measures CO2 levels in exhaled air, assesses airway integrity, and provides a waveform to verify full exhalation. Loss of end-tidal CO2 tracing may indicate airway disconnection or ventilator circuit issues.
Which parameters are closely monitored during initial patient assessment on a ventilator?
-Chest rise, exhaled tidal volume, breath sounds, airway patency and positioning, heart rate, blood pressure, oxygen saturation, and the integrity of the ventilator circuit are closely monitored.
How are ventilator alarms set and why are they important?
-Alarms are set for high and low respiratory rates, low and high minute ventilation, low and high peak pressures, apnea intervals, low PEEP, and low/high end-tidal CO2. They alert clinicians to changes in patient condition, circuit leaks, airway obstruction, or inadequate ventilation.
How often should ventilator parameters and alarm settings be assessed?
-Assessment should occur at least every 3–4 hours, or more frequently depending on patient severity and the frequency of parameter changes. Continuous monitoring of vitals and ventilator parameters is also crucial.
What steps are involved in disassembling a ventilator after patient extubation?
-After extubation, the ventilator is powered down, non-disposable parts like temperature sensors are sent for cleaning, disposable parts are discarded, and the ventilator is wiped down with a cleaning solution before being reassembled for future use.
Why is it important to monitor the shape of the end-tidal capnogram waveform?
-The shape of the waveform confirms complete exhalation. A flattened top indicates full exhalation, while sudden loss of waveform or abnormal shapes may indicate airway disconnection or ventilator malfunction.
What is the significance of setting a low PEEP alarm on a ventilator?
-A low PEEP alarm alerts the clinician to a possible leak in the ventilator circuit or a loss of baseline airway pressure, which is critical to maintain adequate oxygenation and prevent alveolar collapse.
Outlines

Dieser Bereich ist nur für Premium-Benutzer verfügbar. Bitte führen Sie ein Upgrade durch, um auf diesen Abschnitt zuzugreifen.
Upgrade durchführenMindmap

Dieser Bereich ist nur für Premium-Benutzer verfügbar. Bitte führen Sie ein Upgrade durch, um auf diesen Abschnitt zuzugreifen.
Upgrade durchführenKeywords

Dieser Bereich ist nur für Premium-Benutzer verfügbar. Bitte führen Sie ein Upgrade durch, um auf diesen Abschnitt zuzugreifen.
Upgrade durchführenHighlights

Dieser Bereich ist nur für Premium-Benutzer verfügbar. Bitte führen Sie ein Upgrade durch, um auf diesen Abschnitt zuzugreifen.
Upgrade durchführenTranscripts

Dieser Bereich ist nur für Premium-Benutzer verfügbar. Bitte führen Sie ein Upgrade durch, um auf diesen Abschnitt zuzugreifen.
Upgrade durchführenWeitere ähnliche Videos ansehen
Introduction to Mechanical Ventilation by G. Wolf | OPENPediatrics

Anatomy of the Endotracheal Tube (ET Tube) - Airway Management

Ventilator Settings Explained (Mechanical Ventilation Modes Made Easy)

"Chest Tube Placement" by Chris Weldon for OPENPediatrics

ICU Bedside Monitor Tutorial

#3 Les UKMPPD Sistem Pernapasan (Respirasi) - Materi Kedokteran dan Kesehatan
5.0 / 5 (0 votes)
