The Renin-Angiotensin-Aldosterone [RAAS] Pathway EXPLAINED
Summary
TLDRIn this Catalyst University video, Kevin Tockoff delves into the Renin-Angiotensin-Aldosterone System (RAAS), a crucial pathway in health disciplines. He explains how RAAS functions as a negative feedback loop to regulate blood pressure, starting with the release of renin in response to low blood volume or pressure. The video covers the conversion of angiotensinogen to angiotensin II by the lungs' ACE enzyme, which then stimulates aldosterone production to increase blood volume and pressure. Tockoff also touches on the role of angiotensin II in vasoconstriction and hints at upcoming discussions on related medications.
Takeaways
- 🔬 The RAAS system stands for Renin-Angiotensin-Aldosterone System and is a key pathway in health disciplines to regulate blood pressure.
- 🌀 The initial stimulus for the RAAS system is a decrease in blood volume or blood pressure, which triggers a negative feedback loop to raise blood pressure.
- 🧬 Juxtaglomerular cells in the kidney release the enzyme renin in response to low blood pressure, initiating the RAAS pathway.
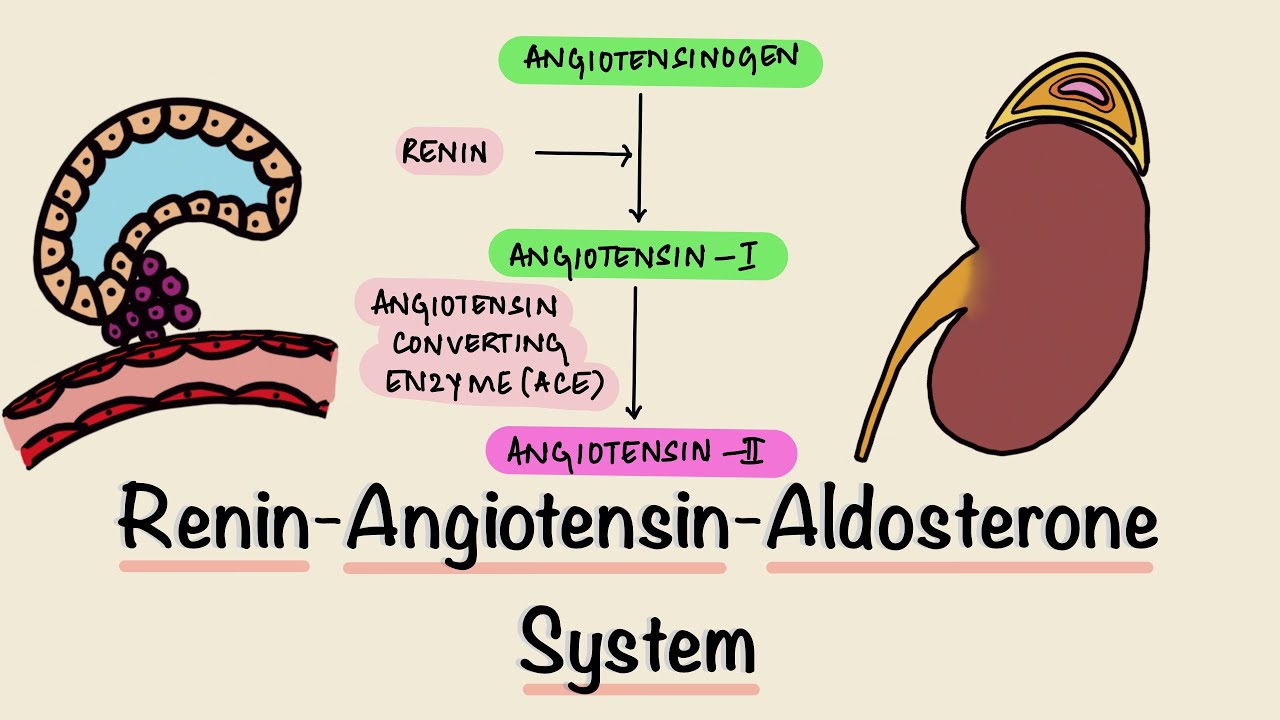
- 🏗️ Renin acts on angiotensinogen, an inactive protein produced by the liver, converting it into angiotensin I, a peptide hormone.
- 💨 Angiotensin I is converted into angiotensin II by the angiotensin-converting enzyme (ACE) in the lungs, which is the active form of the hormone.
- 🚀 Angiotensin II stimulates the adrenal cortex to produce aldosterone, which acts on the kidneys to increase sodium and water reabsorption, thereby raising blood volume and pressure.
- 🔄 The reabsorption of sodium and water due to aldosterone leads to an increase in blood volume, which in turn increases blood pressure, completing the negative feedback loop.
- 🌡️ Angiotensin II also causes vasoconstriction of arterioles, directly increasing blood pressure by constricting blood vessels.
- 💊 Medications such as ACE inhibitors can interfere with the RAAS pathway, providing a method to treat blood pressure issues.
- 🛠️ The understanding of the RAAS system and nephron structure is crucial for comprehending the mechanisms of action of various blood pressure medications.
- 📚 The video promises to cover more on the inhibition of the RAAS pathway and other medications in a subsequent video, highlighting the importance of continued education on the topic.
Q & A
What is the primary function of the renin-angiotensin-aldosterone system (RAAS)?
-The primary function of the RAAS is to regulate blood pressure and blood volume through a negative feedback loop, increasing blood pressure when it is decreased due to low blood volume.
How is blood volume related to blood pressure?
-Blood volume and blood pressure are directly proportional. When blood volume is low, blood pressure is also low, and vice versa.
What is the role of the juxtaglomerular cells in the RAAS?
-Juxtaglomerular cells, located in the kidney, sense decreased blood pressure and release an enzyme called renin into the blood, initiating the RAAS pathway.
What is renin and why is it not considered a hormone?
-Renin is an enzyme, not a hormone, that is released by juxtaglomerular cells in response to low blood pressure. It acts on angiotensinogen to convert it into angiotensin I.
What is the role of angiotensinogen in the RAAS?
-Angiotensinogen is an inactive protein produced by the liver. It is converted into angiotensin I by the action of renin, which is a crucial step in the RAAS pathway.
How does angiotensin II affect blood pressure?
-Angiotensin II is a peptide hormone that acts on the adrenal cortex to stimulate the release of aldosterone and causes vasoconstriction of arterioles, both of which increase blood pressure.
What is the function of aldosterone in the context of the RAAS?
-Aldosterone, released in response to angiotensin II, acts on the kidneys to increase sodium and water reabsorption, leading to an increase in blood volume and blood pressure.
How does the reabsorption of sodium by aldosterone affect water levels in the blood?
-The reabsorption of sodium by aldosterone leads to water following the sodium due to osmosis, resulting in increased blood volume.
What is the significance of the collecting duct in the nephron in the context of the RAAS?
-The collecting duct in the nephron is where aldosterone acts to increase sodium reabsorption and water reabsorption, which in turn increases blood volume and blood pressure.
How do angiotensin-converting enzyme (ACE) inhibitors work in relation to the RAAS?
-ACE inhibitors are drugs that block the conversion of angiotensin I into angiotensin II by the angiotensin-converting enzyme, thus reducing the effects of the RAAS pathway and lowering blood pressure.
What are some potential causes of decreased blood volume that could trigger the RAAS?
-Decreased blood volume can be caused by severe dehydration, sodium deficiency, or bleeding episodes, all of which can trigger the RAAS to restore blood pressure.
Outlines

هذا القسم متوفر فقط للمشتركين. يرجى الترقية للوصول إلى هذه الميزة.
قم بالترقية الآنMindmap

هذا القسم متوفر فقط للمشتركين. يرجى الترقية للوصول إلى هذه الميزة.
قم بالترقية الآنKeywords

هذا القسم متوفر فقط للمشتركين. يرجى الترقية للوصول إلى هذه الميزة.
قم بالترقية الآنHighlights

هذا القسم متوفر فقط للمشتركين. يرجى الترقية للوصول إلى هذه الميزة.
قم بالترقية الآنTranscripts

هذا القسم متوفر فقط للمشتركين. يرجى الترقية للوصول إلى هذه الميزة.
قم بالترقية الآنتصفح المزيد من مقاطع الفيديو ذات الصلة

slide 24

The Renin–Angiotensin–Aldosterone System, RAAS, Animation

Sistema renina angiotensina aldosterona

Renin Angiotensin Aldosterone system

Sistema Renina-Angiotensina-Aldosterona (SRAA) │ MEDICINA RESUMIDA
Renin Angiotensin Aldosterone System | RAAS | Juxtaglomerular Apparatus | JGA | Renal Physiology
5.0 / 5 (0 votes)
